- Author Rachel Wainwright wainwright@abchealthonline.com.
- Public 2023-12-15 07:39.
- Last modified 2025-11-02 20:14.
Subependymal cyst of the brain in a newborn
The content of the article:
- Specifications
- Symptoms
-
Treatment
- Indications for surgical treatment
- Preparing for surgery
- Surgical methods
- Postoperative drug therapy
- Possible consequences
- Forecast
- Video
Subependymal cyst refers to benign brain formations and develops from ependyma (the tissue that lines the ventricles of the brain from the inside).

In the overwhelming majority of cases, the subependymal cyst of the brain does not affect the child's health.
Specifications
It is necessary to differentiate two concepts: pseudocysts and true cystic formations.
| View | Characteristic |
| Pseudocysts | Rather, refer to intrauterine malformations. They have no epithelial lining. Localized under the ependyma of the lateral ventricles of the cerebral hemispheres in the area of the lateral corners of the anterior horns and bodies of the lateral ventricles, as well as in the border area between the head of the caudate nucleus and the optic tubercle. |
| True (arachnoid, retrocerebellar, cerebrospinal fluid) | They have an epithelial lining. As a rule, their appearance is associated with hemorrhages, trauma and other external causes. |
For this reason, the subependymal cyst in a newborn child would be more correctly called a pseudocyst.
Features of pathology:
- The cavity is filled with serous fluid without signs of infection. There are no signs of hemorrhage.
- More often occurs in the tissues of the ependyma of one ventricle, less often in two.
- The wall is formed by a layer of glial cells (the structure is thin-walled, since there is no inner lining).
- It does not have a tendency to grow, since it fills with liquid extremely slowly.
- It has a rounded shape, small size and clear and even contours.
The pathogenesis is based on intrauterine disturbance of the normal development of ependyma in the fetus (cell hyperplasia, slowing down of their differentiation). Various external influences lead to disruption of normal cerebral circulation in the fetus, which leads to hypoxia / ischemia and necrosis of the ependyma areas. This serves as a predisposing factor in the development of a pseudocyst.
Education may have:
- endophytic location - in the wall of the ventricles of the brain at the site of the underdeveloped ependyma;
- exophytic location - over the ependyma with prolapse directly into the ventricular lumen.
Symptoms
This type of neoplasm does not cause significant cerebral disorders and, as a result, the manifestation of symptoms (asymptomatic carriage). More often found as an accidental finding in the diagnosis of pregnant women (planned ultrasound).
If symptoms do occur, it depends on the form, general condition (full-term / premature baby), concomitant diseases (malformations of organs and systems).
Treatment
The subependymal cyst of the brain in a newborn with a small size cannot be treated and does not affect the life and development of the child in any way.
Indications for surgical treatment
An operation to remove a cyst is required in the following cases:
- fast growth;
- serious violations of the outflow of cerebrospinal fluid (development of hydrocephalus);
- suspicion of a malignant tumor (in this case, we are not talking about the degeneration of the subependymal cyst, but about the presence of other formations that were not correctly interpreted);
- significant increase in intracranial pressure;
- convulsive syndrome that cannot be stopped with medication;
- suspicion of hemorrhage.
Typical signs of hydrocephalus:
- an increase in head volume in a short period of time;
- pulsation and bulging of fontanelles;
- divergence of the bones of the skull, which leads to a visible deformation of the head;
- lag in psychological development as a consequence of ischemia of brain tissue under constant fluid pressure.
Preparing for surgery
Preparation for surgery includes the following studies:
- general analysis of blood and urine;
- coagulogram;
- blood chemistry;
- determination of blood group and Rh factor;
- Ultrasound;
- CT / MRI.
Surgical methods
| View | Operation stages |
| Ventriculoperitoneal shunting |
Used when symptoms of hydrocephalus occur. The essence of the operation is to create a kind of system between the ventricles of the brain and the abdominal cavity in order to drain excess cerebrospinal fluid. This is achieved using special silicone catheters. When placing a shunt, as a rule, neurosurgeons and pediatric surgeons work at the same time. Stages: 1. The operation is performed in the area of the temporal bones (right or left at the Kocher point). The tissues are dissected in layers, then the bones of the skull are separated (not completely, leaving a nutritive leg on one side of the wound). With the help of a ventricular catheter, the ventricular system is punctured. 2. In this case, pediatric surgeons, using laparoscopic techniques, enter the abdominal cavity (access to the peritoneum). Further, with the help of a shunt-passer (special conductor), a stroke is made in the subcutaneous fatty tissue up to the trepanation hole (it passes through the subcutaneous tissue of the abdominal wall, chest wall, neck and part of the skull). 3. The two systems are connected at the burr hole: the distal part of the catheter, which extends from the peritoneum, and the ventral part of the catheter, which exits the ventricles of the brain. 4. The system is checked for consistency (no leakage of cerebrospinal fluid, twists or bends). 5. The fabrics are tightly sutured in layers. Periodic monitoring of the shunt condition is required. |
| Endoscopic intervention (ventricular endoscopy). |
It is carried out using special high-tech equipment. This technique is optimal for cystic formations, the complete excision of which is impossible due to the deep location. With the help of an endoscope, surgeons get a visual picture of the inner cavity of the brain ventricles. This allows you to determine the exact location of the cyst and the nature of the hydrocephalus (occlusive). The surgeon makes a hole in the skull bone through which an endoscope will be introduced, with which the cyst wall is incised. Thus, its cavity is connected to the cerebrospinal fluid system (a special version of the drainage of the formation). Endoscopic ventriculocisternostomy of the fundus of the third ventricle is most often performed. In this case, all the fluid from the third ventricle is excreted into the brain cisterns. |
| Craniotomy. |
The most traumatic type of surgery. It is extremely rarely used for this type of pathology, since this method is more suitable for superficial formations. Stages: 1. Layer-by-layer dissection of skin tissue and subcutaneous fatty tissue, aponeurosis up to the bones of the skull. 2. Using a special tool, holes are made in the bone. 3. The bones between the holes are filed and separated, exposing the brain area covered with membranes. 4. The membranes are carefully incised and gradually pass into the depths until the cyst is detected. 5. Complete or partial excision of the cavity is performed with sending the biomaterial for cytological or histological examination. 6. The wound is sutured in layers, and the bones of the skull are fixed with titanium plates. |
Postoperative drug therapy
The course of drugs in the postoperative period includes:
- Anticoagulants for the prevention of thrombosis. These include Heparin, Antithrombin.
- Immunomodulators to support the immune system as it is imperfect in newborns. Group drugs include cytokines, Interferon.
- Antibacterial or antiviral agents for the prevention of infection - Cefepim, Azithromycin.
- Nootropics to restore brain function - Nootropil.
- Antioxidants and vitamin complexes to restore metabolic processes in tissues.
If necessary, the postoperative period includes infusion-detoxification therapy (physiological solutions, Ringer's solution, glucose).

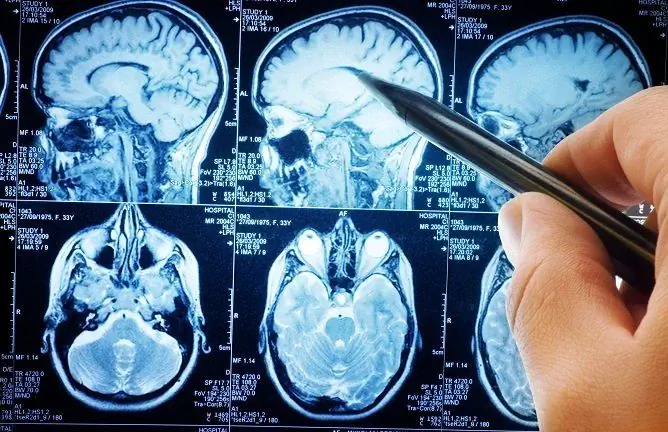
Neurosonography, or ultrasound of the brain, is the main method for diagnosing cerebral cysts in children
Possible consequences
Consequences arise in the event of complications (rupture, suppuration, hydrocephalus) or after surgery:
- Lagging in mental and physical development (delayed speech, memory impairment). It does not occur immediately, but as the child grows up to 2-3 years. This complication is caused by prolonged compression of the brain tissue and irreversible changes in the cerebral cortex. It manifests itself in varying degrees (with mild disorders, they will not interfere with normal life).
- Epileptic seizures. They arise as a result of reflex trauma to the brain tissue (violation of nerve conduction in a separate part of the brain). Status epilepticus is rare.
- Bleeding with the formation of hematomas in the cavity of the ventricles or in the substance of the brain. A formidable complication, which in some cases requires reoperation and removal. Total hemorrhage (stroke) rarely occurs in children.
- Swelling of the brain. Occurs in case of damage to the water supply of the brain. In this case, the CSF ducts may become clogged, and hydrocephalus occurs, but already as a secondary phenomenon. A complication requires immediate treatment, since with damage to the medulla oblongata, respiratory arrest or cardiac arrest may occur.
- Accession of infection with the occurrence of abscesses, encephalitis or meningitis. In this case, a mandatory course of antibiotics in the postoperative period is indicated.
- Focal symptoms (loss of visual fields, hearing impairment, loss of sensitivity). The manifestations will depend on the specific area that was traumatized during the surgical intervention.
Complications are relatively rare.
Forecast
Both pediatricians (for example, the famous doctor Komarovsky) and neurologists give a favorable prognosis in 90-95% of children with this pathology.
Video
We offer for viewing a video on the topic of the article.

Anna Kozlova Medical journalist About the author
Education: Rostov State Medical University, specialty "General Medicine".
Found a mistake in the text? Select it and press Ctrl + Enter.