- Author Rachel Wainwright wainwright@abchealthonline.com.
- Public 2024-01-15 19:51.
- Last modified 2025-11-02 20:14.
Hernia of the lumbosacral spine
The content of the article:
- Features:
- Kinds
- Symptoms of a hernia of the lumbosacral spine
-
Treatment
- Conservative therapy
- Surgery
- Video
A hernia of the lumbosacral spine is a protrusion of part of the intervertebral disc due to rupture of the annulus fibrosus. Displacement occurs towards the spinal canal. Most often, hernias occur in the lumbar region, since this part of the spinal column has the maximum load. Also, this section of the spine has a greater height of the intervertebral discs than other sections, and a weak longitudinal ligament, which normally provides fixation of the vertebrae along the anterior and posterior surfaces.

In the lumbosacral spine, hernias occur more often than in other parts
Features:
Features of the intervertebral hernia of the lumbosacral region:
- occurs more often in middle-aged people;
- is the main cause of pain in the lumbar region;
- the first signs of the disease can occur from the lower extremities (numbness of the legs, impaired motor activity);
- the main diagnostic method is X-ray (a hernia is designated as a protrusion between the vertebrae);
- amenable to conservative treatment in 75% of cases;
- the main cause of the occurrence is trauma to the spinal column (weight lifting, professional sports).
The sacrum is involved in the pathological process less often than the lower back (structural features). For this reason, hernias occur at the L5-S1 level in 50-55% of cases, at the L4-L5 level in 25-30% of cases (L - designation of the lumbar vertebrae, S - sacral). According to ICD 10, pathology is indicated by the letter M (M 51.0; M 51.3; M 52.1; M 52.2)
Kinds
Depending on the anatomical location of the hernia in relation to the spinal canal, there are:
| View | Features: |
| Median or median |
Refers to internal, since it is located in the center of the intervertebral disc and, accordingly, causes compression of the internal roots. In the clinic, radicular syndrome often dominates over local manifestations. |
| Paramedian |
The specific location explains the simultaneous compression of two nerves - the inner root and the outer one that emerges from the spinal cord. The clinic is represented by both local and radicular syndromes. |
| Posolateral or lateral |
Only the outgoing nerve root is involved in the lesion, since the hernial protrusion is located in the lateral area and squeezes all structures of the outer edge of the disc. More often, only local manifestations of pathology occur, radicular symptoms are either mild or absent. |
Depending on the degree of destruction of the annulus fibrosus and other elements of the intervertebral disc, the following types of pathology are distinguished:
- Disc protrusion. It is manifested by the displacement of the elements of the intervertebral disc directly into the spinal canal. As a rule, the very structure of the disk is not disturbed.
- Extrusion. In this case, the annulus fibrosus breaks and the nucleus protrudes into the spinal canal. At the same time, the posterior longitudinal ligament is preserved.
- Prolapse. It is associated with the prolapse of the altered components of the annulus fibrosus directly into the spinal canal.
- Sequestration is a process associated with the displacement of fragments of the annulus fibrosus along the spinal canal (continuation of prolapse).
Symptoms of a hernia of the lumbosacral spine
Symptoms will depend on the location of the hernia, since various nerve endings are compressed with one or another location of the formation.
There are two categories of symptoms: local and radicular.
| Symptoms | Cause of occurrence | Clinic |
| Local |
May be due compression of the outgoing branches of the spinal nerves, violation of the integrity of the articular apparatus, damage to the intervertebral disc. |
Low back pain is the main symptom. At the onset of the disease, with small sizes of hernias (less than 1-2 mm), it is slightly expressed. The intensity gradually increases as the disease progresses. Irradiation of pain to adjacent areas (thigh, buttocks) as it progresses. A clear dependence of the pain syndrome on physical activity, even insignificant (increased pain when coughing, sneezing). Local changes in the form of hyperemia, edema or visible deformation are not observed. |
| Radicular | It occurs when the hernia protrudes towards the spinal canal. |
Violation of the sensitive innervation of the extremities (tingling and goose bumps in the feet, legs). Violation of motor activity (paresis). Cauda equina syndrome, which is associated with damage to a large area of the spinal cord. It manifests itself, in addition to disorders of the motor and sensory spheres, dysfunction of the pelvic organs. Since each part of the spinal cord is responsible for the innervation of its own area, the clinic will depend on the level of damage (L1-L5, S1). |
Symptoms are typical for a number of other diseases (radiculitis, osteochondrosis), which somewhat complicates the diagnosis and sometimes requires additional examination methods (MRI / CT).

The clinical picture depends on the level at which the damage occurred
Treatment
In most cases, a hernia of the lumbosacral spine is treated without surgery, since surgical intervention in this anatomical region has a high risk of complications.
Conservative therapy
- Bed rest for 5-7 days in order to stop degenerative processes in tissues.
- Analgesics (Drotaverin) to relieve pain. Paravertebral blockade with lidocaine solution almost completely relieves pain syndrome, but has a high risk of complications.
- Non-steroidal anti-inflammatory drugs for the relief of concomitant aseptic inflammation in the surrounding tissues of the back (Diclofenac, Ibuprofen).
- Muscle relaxants for relieving reflex muscle spasm (Vecuronium, Pancuronium).
- Exercise therapy. A strictly individually special set of exercises is selected. It can act as part of conservative therapy, or as part of the rehabilitation period after surgery.
- Physiotherapy procedures. The specific type of treatment (electrophoresis, magnetotherapy, cryotherapy, UHF therapy) is prescribed by the doctor. It can also be used both in the preoperative and postoperative period.
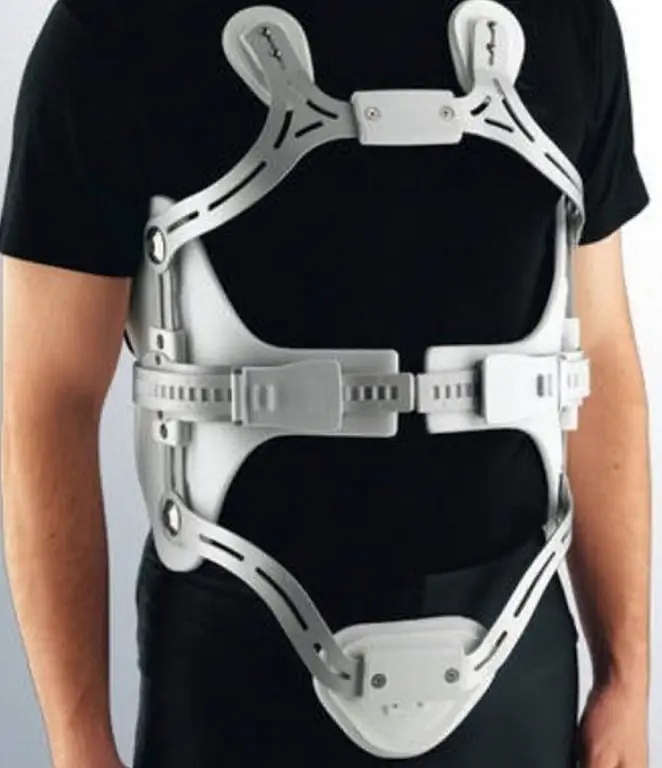
- Special orthopedic accessories (corsets, bandages). Stiffness and type are selected taking into account the nature of the hernia.
It is permissible to treat a person using conservative methods in the case of an insignificant hernia and the absence of pronounced destruction of bone structures.
Surgery
The goal of the surgery is to decompress the spinal nerves.
Indications for surgery:
- duration of radicular syndrome more than 4 weeks (loss of nerve function);
- lack of effect from conservative therapy;
- MRI signs of hernial protrusion.
Contraindications to surgery:
- instability of the spinal segment;
- narrowing of the spinal canal;
- the presence of growths and osteophytes in the projection of the spinal canal;
- signs of spondylosis.
Options for operational tactics:
| Method | Description |
| Intralaminar microdiscectomy using an operating microscope | The method belongs to high-tech, since it requires magnifying devices (forehead magnifier, operating microscope). It allows you to remove a hernial formation of almost any location and size. During the operation, there is minimal blood loss and minimal tissue trauma (high cosmetic quality). The average stay in the neurosurgical department is 5-7 days. After the operation, a rehabilitation course is indicated and after 6 weeks, full physical activity returns. In the postoperative period, wearing a corset and limiting physical activity to 3 months is indicated. |
| Microendoscopic discectomy | It is a muscle-dividing operation and refers to endoscopic methods of surgical intervention. Special equipment is used to visualize the operating field (endoscope). It is used for hernias located laterally, osteophytes in the canal cavity. It is unacceptable to use this method for repeated spinal surgery. Intralaminar access only. The patient is discharged for 3-4 days, and the rehabilitation period is reduced to 4-5 weeks. |
| Percutaneous endoscopic lumbar discectomy | It is carried out using an endoscope and other specialized instruments. It is possible to introduce equipment using three approaches: intralaminar, posterolateral, and transforaminal. It is used for typical unchanged hernias. The patient is discharged for 3-4 days, and the rehabilitation period is reduced to 4 weeks. |
Any surgical intervention is accompanied by a risk. Complications arising during the operation include:
- Bleeding. They occur relatively rarely when the central vein is damaged. Shows immediate hemostasis. As a rule, blood loss does not exceed 150-200 ml of blood.
- Damage to the structures of the spinal canal (in particular, the membranes of the spinal cord). In this case, CSF leakage occurs. With the development of liquorrhea, special sealing seams and an adhesive substance are applied over them.
- Damage to the nerve roots. It is relatively rare. If the distance between the crossed sections of the nerve does not exceed 1.5 cm, special sutures are applied. Despite the stitching of the nerve fiber, there is a risk of dysfunction of this nerve in the postoperative period.
Postoperative complications include:
- Recurrent hernias. The operation in this case will be required only if there are clinical manifestations (radicular syndrome).
- Accession of a secondary infection and wound suppuration.
- External wound liquorrhea (damage to the dura mater during surgery). To stop, use a special agent consisting of fibrin and thrombin.
Complications occur in a very small percentage of people, since minimally invasive surgical methods are the gold standard in the treatment of intervertebral hernia of the lumbosacral spine.
Video
We offer for viewing a video on the topic of the article.

Anna Kozlova Medical journalist About the author
Education: Rostov State Medical University, specialty "General Medicine".
Found a mistake in the text? Select it and press Ctrl + Enter.