- Author Rachel Wainwright wainwright@abchealthonline.com.
- Public 2023-12-15 07:39.
- Last modified 2025-11-02 20:14.
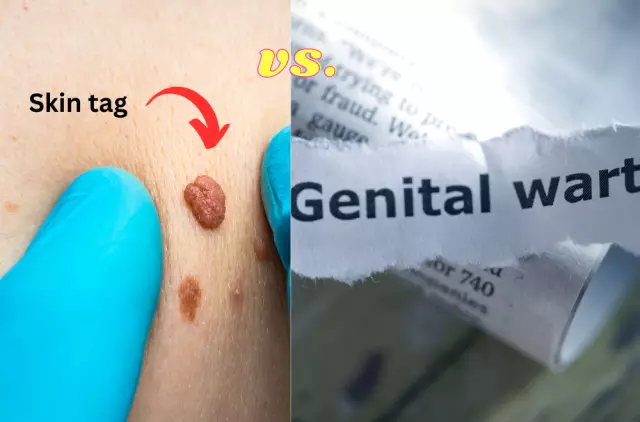
New treatment options for genital warts
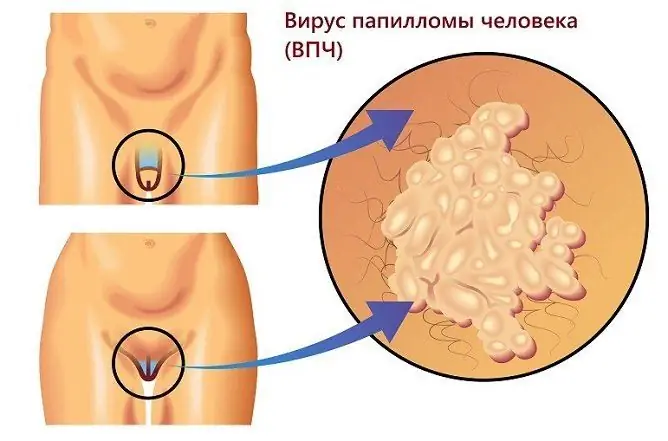
To date, we do not reliably know the exact number of people infected with the human papillomavirus. Nevertheless, we know that in every seventh, this disease manifests itself in the form of genital warts, the risk of which is highest among those who are sexually active.
The sexually transmitted human papillomavirus is dangerous not only as the cause of genital warts, but as one of the factors in the development of oncological diseases such as cervical cancer and penile tumors. Thus, genital warts are not only a cosmetic defect, but also a marker of infection with a dangerous virus, some of the strains of which can cause the development of malignant neoplasms.
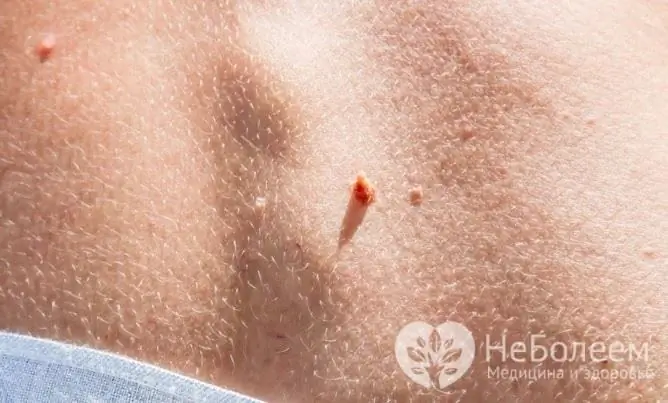
Today, there are various types of treatment for genital warts. These methods can be divided into two large groups - destructive and conservative methods. Among the destructive techniques, in addition to surgical treatment, one can single out procedures aimed at the destruction of genital warts using physical or chemical factors. Within the framework of conservative methods of therapy, drugs are widely used, the purpose of which is to stimulate the methods of natural nonspecific defense of the body.
Although destructive methods allow you to quickly get rid of genital warts, their use may require the use of specialized, expensive and sometimes extremely difficult equipment to control, requiring the involvement of trained highly qualified personnel and the use of various anesthetic techniques. The use of destructive methods is accompanied by the development of pain in the patient, both during the procedure and in the early postoperative period.
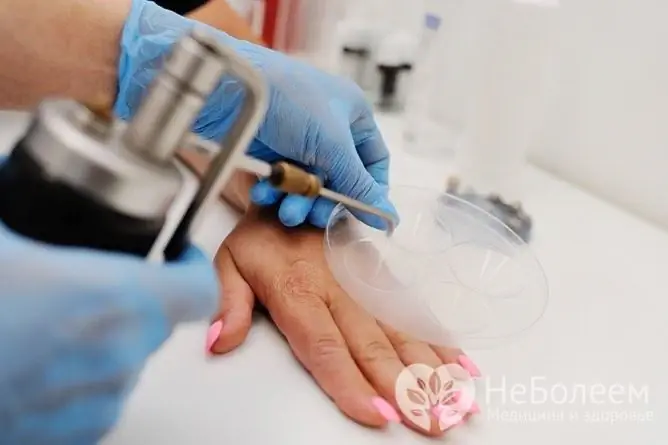
And when using concentrated solutions of acids, without observing proper safety precautions, they can get on unaffected skin, mucous membranes, eyes.
It is important to emphasize that the removal of genital warts is only the elimination of a visible symptom and does not mean the elimination of the human papillomavirus from the body. Therefore, after the use of destructive methods of treatment, there is always a risk of recurrence of the disease.
As a prevention of recurrence of genital warts in the postoperative period or after topical application of aggressive chemical compounds, it is necessary to prescribe drugs that stimulate the body's own protective factors, aimed at suppressing HPV activity.
Such drugs are the basis of conservative etiopathogenetic therapy for genital warts, and in some cases are the only effective treatment.
The functioning of the links of immunity is based on the pathogen recognition system, which in a simplified form can be described as "friend or foe". To identify foreign agents on the surface of the membrane of immunocompetent cells and on intracellular structures, there are specific protein structures that function as receptors. The role of Toll-like receptors, discovered in 1996, was the recognition of the molecular pattern of the pathogen, signal transmission into the cell and, as a consequence, the activation of the mechanisms of nonspecific immune defense of the body.
For this discovery in 2011, the French immunologist Jules Offman, together with the American physician Bruce Boettler and the Canadian cytologist Ralph Maine Steiman, were awarded the Nobel Prize in Medicine.
In 1997, preparations were created based on the active ingredient imiquimod or imiquimod, interacting with Toll-like receptors on the cell surface and, thus, stimulating the body's nonspecific immune response.
Currently, drugs of this group are widely used for the treatment of genital warts, as well as in oncology for the treatment of basal cell and squamous cell skin cancer.
In addition to its high efficiency, proven in numerous (more than 2500) clinical studies, the advantages of imichimod include the convenience and safety of its use, which allows the patient to use it independently, at home, without wasting time and money for additional visits to the doctor.
For a long time, the use of these drugs was limited by their rather high cost, however, in 2015, a drug based on imichimod began to be produced in the Russian Federation, which made it possible to reduce its cost and thereby increase its availability.
Found a mistake in the text? Select it and press Ctrl + Enter.